Inside the ‘miracle’ drug rollout that might finish Aids | EUROtoday
Lianne was simply 13 when she misplaced her dad and mom to Aids. Newly orphaned, she needed to discover a strategy to preserve herself and her youthful sister alive. With no cash to complete faculty, unable to discover a job and struggling to place meals on the desk, there was just one possibility – intercourse work.
Now 24, she is aware of the hazards in Eswatini, a kingdom in southern Africa as soon as described because the epicentre of the HIV epidemic and a rustic nonetheless combating among the highest an infection charges on the earth.
“Both my parents passed away. Hunger led me to join this work although I know it’s risky,” Lianne says, explaining that she earns underneath £25 per week. She is unable to amass HIV preventative medicine – often known as PrEP – on her personal.
But there may be now hope within the type of lenacapavir – dubbed the “miracle” drug – which the United Nations hopes can defend tens of millions of individuals like Lianne and even finish the Aids epidemic altogether.
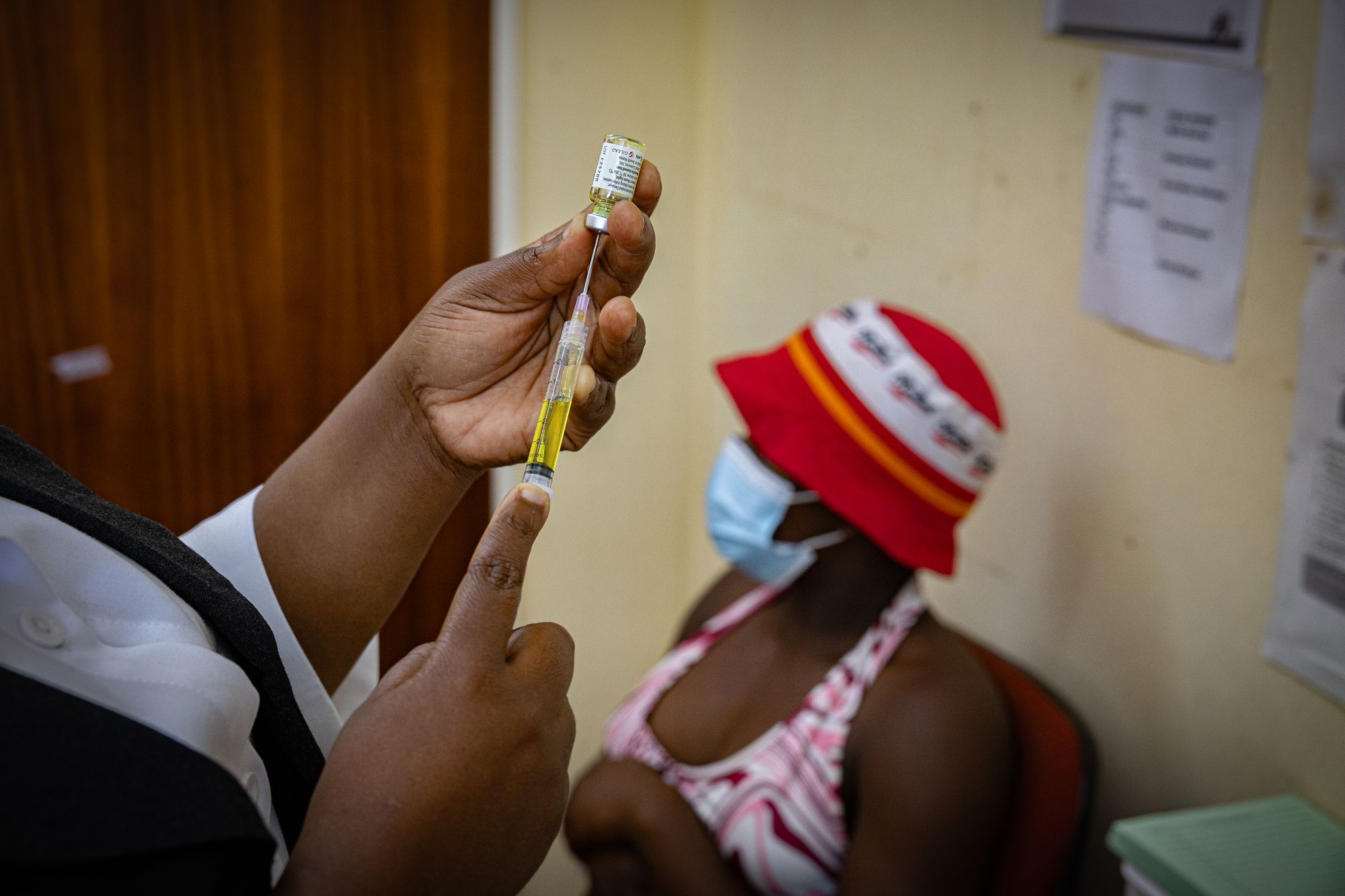
The twice-yearly injection – described by the top of the UN Aids company as “the closest thing we have to a vaccine” – supplies close to full safety in opposition to an infection.
Lenacapavir is being launched for the primary time in 9 of essentially the most at-risk nations, together with Eswatini, that means Lianne was among the many first folks on the earth to get the injection.
While it’s a huge step ahead in HIV care, issues have been raised concerning the extent of the rollout and fears will probably be ineffective if it’s not launched on a worldwide scale.
The optimistic information about lenacapavir comes after final 12 months’s devastating cuts to international assist spending by US president Donald Trump, which had beforehand funded round half of Eswatini’s HIV response.
For Lianne, it meant the abrupt closure of the cell clinics that gave her entry to doubtlessly life-saving HIV prevention remedy without cost.
The closures have had a lethal impact: a buddy and fellow intercourse employee just lately died after contracting HIV and dropping entry to life-sustaining medicine.
“That is why I am so happy today, it’s protection,” she continues with aid, as she receives the brightly colored yellow injection.
At the start of 2025, the world was on monitor to finish the Aids pandemic by 2030.
But that was upended by unprecedented international assist cuts from the US, the UK and different European nations, which have created the most important ever disruptions to HIV response, from testing to therapy and prevention.
If these assist cuts proceed, there may very well be tens of millions extra deaths and infections, in addition to double the variety of medication-resistant strains, based on The Independent’s personal modelling of information.
This makes the timing for the lenacapavir rollout important. Developed by California-based biopharmaceutical firm Gilead Sciences, the UN believes the therapy, if correctly deployed, might assist convey concerning the finish of the epidemic by decreasing new infections to zero.
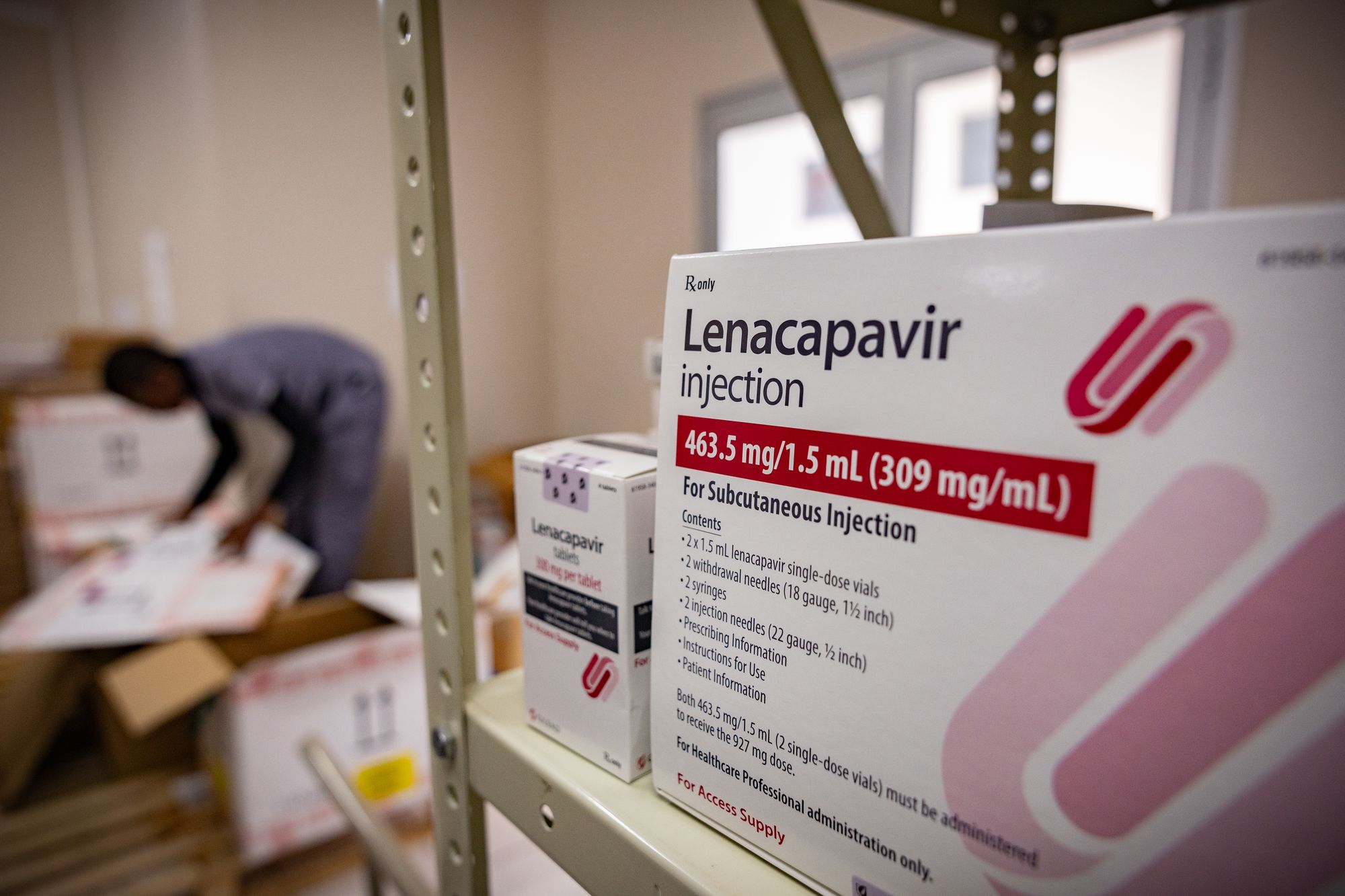
The present plan, funded by the Global Fund to Fight Aids, TB and Malaria, along with the US authorities and others, is to ship lenacapavir to 3 million folks by 2028.
Lenacapavir, which in rich nations can value as much as $24,000 (£18,000) a 12 months, is being concurrently delivered to among the poorest nations most in danger at a considerably lowered value.
Life-sustaining antiretroviral remedy was infamously accessible within the West for a full decade earlier than being rolled out in sub-Saharan Africa, costing numerous lives and paving a approach for the disaster as we speak.
“This has been a defining moment for the Aids epidemic,” says Dianne Stewart from the Global Fund. “We have been fighting for equitable access to new tools since the beginning, and this is the first time in history that we have got it right.”
The first nation to obtain these jabs is Eswatini. Formerly often known as Swaziland, it has labored onerous to cut back new HIV infections from a peak of 21,000 per 12 months 20 years in the past to 4,000 in 2023, based on the UN.
But nonetheless round 1 / 4 of Swazis aged between 15 and 49 live with HIV, based on the most recent knowledge from the US Center for Disease Control.

David Maseko of HealthPlus for males, a charity working with key populations together with LGBT+ communities, explains that the help cuts shut all 15 cell charity clinics that Lianne and others used.
That has meant there was a hovering variety of folks – together with among the most at-risk communities – off their HIV medicine and off PrEP – an issue unfolding throughout Sub-Saharan Africa.
“There are a lot of gaps now. We are even struggling to do community testing.”
For him, a twice-yearly injection that might assist curb the current surge in infections is “simply a game-changer”.
Arianna, 17, who was additionally compelled into intercourse work after her mom died and she or he left an abusive residence, agrees. “This is lifesaving for us,” she says as she will get the injection.
She explains that making an attempt to get day by day prevention PrEP tablets from a public facility, the place she might face prejudice as a intercourse employee, makes it close to unattainable, particularly after they earn so little per week to cowl transport.
“That is why today I decided to come here. To me, this is the best way to help myself, to survive.”
But there are issues that with out correct funding around the globe to achieve a important mass of individuals protected globally, the impression will probably be restricted.
For now, supply is focused at simply 9 nations, though there are plans to broaden that. Lenacapavir has not but been licensed or procured for supply in massive elements of Latin America, the place an infection charges are rising.
“We have seen in the past that piecemeal solutions, especially for infectious diseases, do not work,” provides Stewart from the Global Fund.
“As we saw during Covid, you cannot solve it in one country and think it is done while others do not have access.”
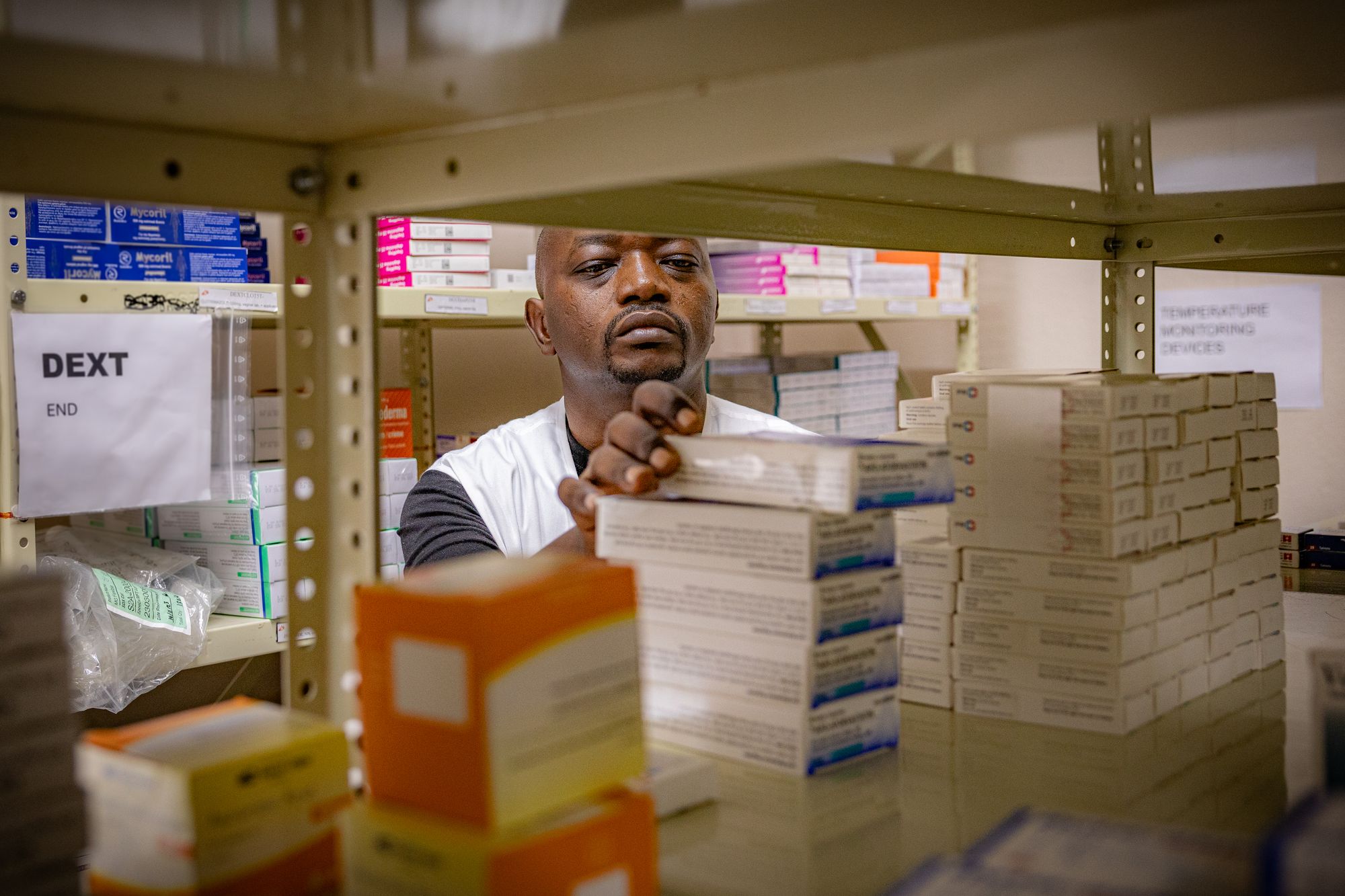
At a Medecins Sans Frontieres (MSF) clinic in a city exterior the capital, nation lead Dr Diojki Bahati says they got solely 50 doses to distribute and have needed to flip sufferers away.
Even reaching two million folks with lenacapavir over the subsequent three years is “far below the global need”, he continues.
UNAIDS has stated that to deal with the pandemic, the world must get 20 million folks on PrEP within the subsequent few years.
“Two million people over three years is less than 10 per cent of that target.”
He provides that there are not any various procurement methods, particularly for organisations like MSF, that he says have been denied the proper to buy instantly.
In parallel, generic manufacturing licences have been granted to round six producers within the coming 12 months to produce 120 nations and territories.
“But that leaves quite a number of low- and middle-income countries where up to 20 per cent of new infections are happening,” he continues, akin to Brazil, Peru and Mexico that participated in lenacapavir drug trial.
He says it’s important that the rollout is correctly funded and supported by governments, whilst they lower assist. It will finally be significantly cheaper in the long run.
In 2024, there have been no less than 1.3 million new HIV infections. Carmen Pérez Casas, from well being initiative Unitaid, explains that these further infections will value an additional $52m (£38.8m) per 12 months if everyone seems to be placed on antiretroviral therapy, resulting in a lifetime therapy value of roughly $2bn.
As transmission will increase, this value will accumulate exponentially over time.
“This is a fraction of what it could cost to deliver lenacapavir … at the scale required to bend the curve of the epidemic,” she provides.
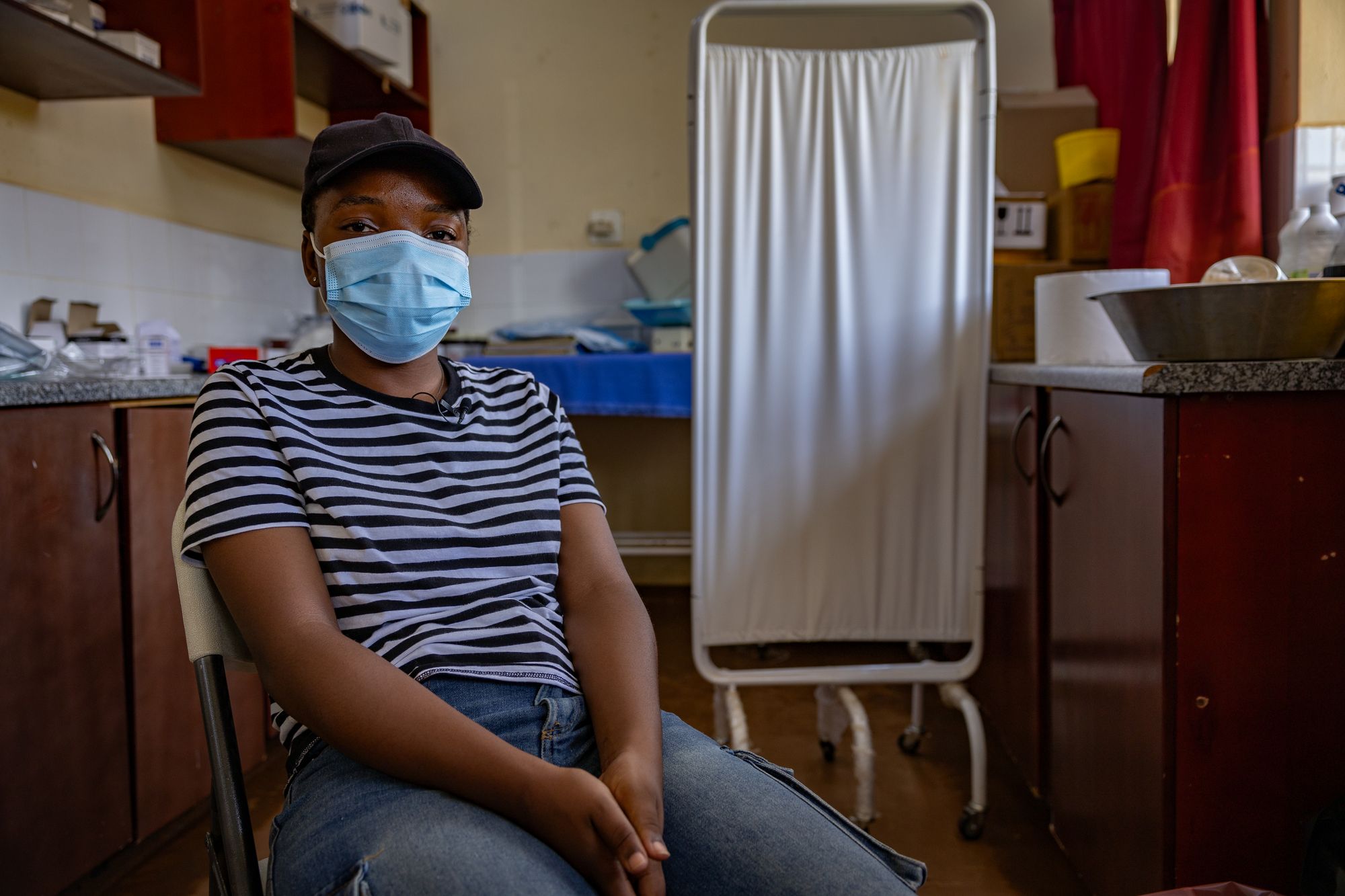
Back within the Eswatini clinic, the demand is clearly there. Lianne and Arianna breathe a sigh of aid after getting their jabs, understanding for now they’re protected.
“We beg that they do not get tired of helping us,” says Lianne as she finishes her appointment. “If they are cutting the funding, it means we will be exposed and die of HIV. Please help.”
This article has been produced as a part of The Independent’s Rethinking Global Aid undertaking
https://www.independent.co.uk/news/world/africa/hiv-lenacapavir-eswatini-aid-cuts-aids-b2942293.html
